A Candid Report on My Trip to Planet Postpartum

I think everyone who gives birth leaves Earth for awhile to visit another planet. Time does not exist there. The days bleed into one another, swathed in the relentless and bleary-eyed fog of new parenthood. That fog is everything the proverbial “they” say it is—a mish-mash of wonder, love, fear, delight, overwhelm, sleep deprivation, tidal waves of hormones, physical pain, emotional reckoning, and moments of feeling absolutely incompetent.
As with many things, comparison can be the thief of joy. I think about this pretty much every time I share something on social media or any time I’ve tried to write something real about my postpartum experience. How do I share authentically without triggering someone who is childless/childfree, but not necessarily by choice? Or, alternatively, someone who is a parent, but not necessarily by choice? Or a parent whose journey has been more tumultuous than my own?
On the other side of the coin, how do I talk about challenges I’ve experienced with candor and vulnerability, but without being whiny, petty or, worst, ungrateful—for a child in the first place, for a wonderful partner, for many extraordinary privileges, for access to healthcare, for paid parental leave from my job, for the incredible support of our friends, family and community throughout such an already-weird year?
I confess I’ve been posting photos and videos of Sahale often on social media because (a) it can otherwise be lonely to raise a baby in the relative isolation of a global pandemic (what I would give for my parents to be able to meet and hold their grandchild!), and (b) I hope she can still bring genuine joy to friends and family far away—even as I recognize that babies can also be a source of pain for anyone grappling with infertility, miscarriage, stillbirth, or what’s often called “childlessness by circumstance.”
Additionally, how do I share what might be of value to other new (or soon-to-be) parents without going TMI on those who aren’t interested in the particulars of childbirth recovery?
I’m not sure, but if you’re still here, buckle up for the ride. Here are three months’ worth of experiences and reflections on my time so far on Planet Postpartum.
Birth by Planned C-Section
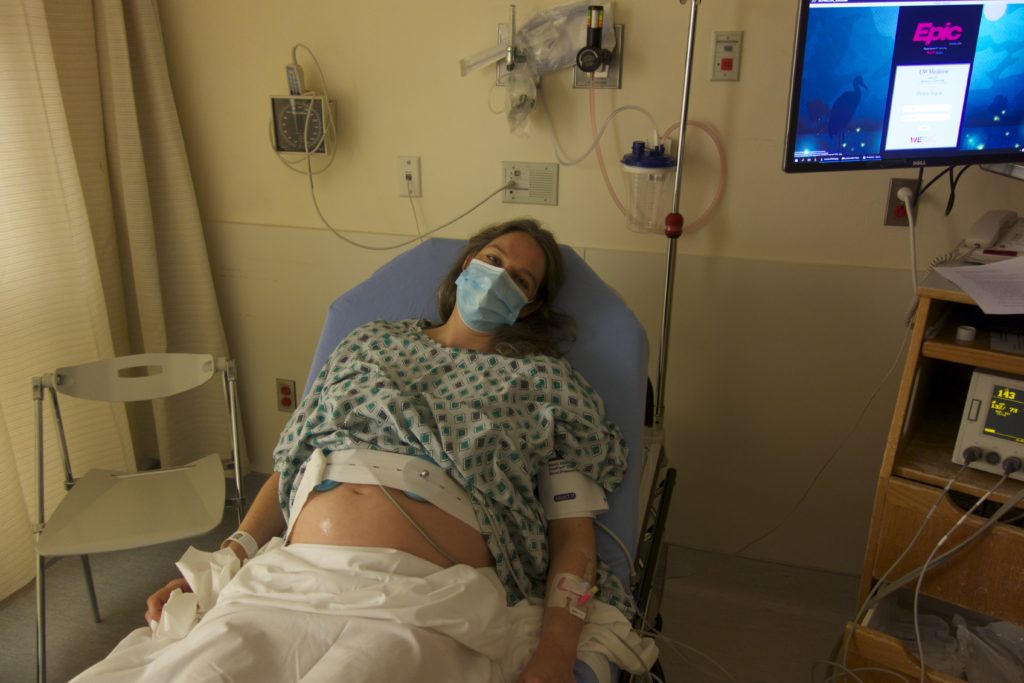
First of all, I’m incredibly grateful to the many people in my life who’d already paid a visit to this planet—fellow parents, runner mamas, and especially anyone who’s had a C-section—and helped me sketch out a little itinerary. Of course, I didn’t expect to wind up having my baby via C-section. (Does anyone? Probs no.) This was the first heartbreak—the news at 36 weeks that our baby was breech. Over the next three weeks, as it became increasingly obvious that she wasn’t going to do any somersaults in the womb, I moved rapidly through all five stages of grief over the loss of the natural birthing experience I’d imagined.
Denial: “Maybe she flipped last night and that grapefruit under my ribcage is actually her butt, not her head.”
Anger: “$&#@, I don’t want abdominal surgery!”
Bargaining: “Let me meditate/stretch/pray/invert/massage/chiropract my way out of this.”
Depression: “Why meeee?”
Acceptance: Schedule surgery, google “C-section birth plans,” realize that a Cesarean—especially when planned, rather than emergent—is not actually the horror-fest worst-case scenario that all the books I’d read and the HypnoBirthing classes we’d taken on Zoom had made it out to be. In all honesty, I found it to be a pretty lovely way for Sahale to enter the world. I even got to snuggle with her on my chest while they sewed me back up.

As I’m writing this, I can hear in myself the same whiff of defensiveness that so many new parents seem to feel obligated to wield when sharing that they’ve deviated from whatever baby-related gold standard we’ve all been told is critical to the long-term health, happiness and intelligence of our offspring. (Economist Emily Oester does a decent job unraveling some persistent myths about pregnancy, birth and infancy in her books Expecting Better and Cribsheet.) Part of me felt like I’d somehow “cheated” after padding into an operating room in my socks one Thursday morning and getting wheeled out less than an hour later with a baby in my arms and an intact vagina.

The other part of me was too busy swimming in euphoria to dwell on the fact that she came out the skylight instead of through the front door.
Other than not sleeping for the next 50 hours, filling a literal bucket with bloody discharge (lochia) every time I peed, getting hickeys all over my breasts from dozens of poorly aimed latching attempts, and fretting needlessly over tests (jaundice, hearing impairment, etc.) that Sahale initially failed but which, it turns out, are prone to false positives … other than all that, our hospital stay was just fine. Our nurses were great. There are some upsides to giving birth in a pandemic; personally, I loved not having visitors in the hospital and being able to bond so intensely with George and Sahale for the first two days of her life.

I didn’t quite realize what terrific painkillers I’d been loaded up with during and after surgery; I took slow but painless walks up and down the hospital hallway that first night, gleeful that I felt so awesome, and deluded into thinking I’d continue to feel that way.
The Initial Haze + Breastfeeding Woes

Then I got home. George was amazing during this time, but nevertheless, the realities of recovering from major surgery while also managing the steep learning curve of caring for an infant set in. For me, breastfeeding was the steepest learning curve of all. Sahale failed to gain enough (OK, any) weight in the second week of her life because, basically, neither she nor I had any idea what we were doing; plus, the combination of her high palate and my dainty nipples made achieving a good, milk-transferring latch all the more of a challenge for us.
Oester summed it up well when she wrote about the common experience of medical professionals’ consternation if your newborn fails to gain weight rapidly enough: “When you’re just postpartum and trying to breastfeed for the first time, this can be a very fraught conversation. It can feel like you are failing—you did such a great job growing this baby inside you, and now that it’s out, you totally suck. (You don’t! That’s just how it feels.)”
We enlisted the help of lactation consultants (LCs) at the hospital—but these were a mixed bag, providing useful guidance but also creating some additional stress. The only thing more painful than the spinal injection before my C-section was the LC who attempted to evert my inverted nipple by pinching it like a cockroach she was intent on squashing the life out of.
I’m sure everyone’s C-section recovery is different, but the early weeks were not fun. (From what I hear, vaginal birth recovery can be just as not-fun … just in different ways.) My incision got infected almost immediately, I didn’t poop for six days, and around-the-clock Tylenol and ibuprofen weren’t enough to staunch excruciating pain in my left hip. Even after a couple weeks, my hip hurt so much that I could barely walk around the block. My body felt so foreign and broken that I told George I was concerned they’d accidentally left a medical instrument jammed into the left side of my pelvis when they sewed me back up. (It’s good that he and I have paced at each other at so many ultras, so are accustomed to talking down one another’s hyperbolic theories about bodily woes.)
At first, I couldn’t go up or down any stairs, get myself in and out of bed, or even stand up from the toilet on my own. If I managed to find time and energy to shower every other day, it felt like a real accomplishment. During this time, George brought me coffee and breakfast in bed every day, changed all of Sahale’s diapers, and did everything around the house for us while I basically stayed in our bedroom icing my hip, eating Percocets, marveling at our baby, and gritting my teeth while she chomped on my bruised and cracked nipples for eight to ten hours a day. Our latch was so bad that she was struggling to get enough milk, so she often nursed for over an hour at a time just trying to fill her poor little cherry-sized stomach. I was so exhausted that I could scarcely stay awake during the endless cycle of feedings.

A week and a half into her life, I swapped out breastfeeding for pumping milk around the clock to increase my tanked supply, let my nipples heal, and know exactly how much milk Sahale was getting at each feed. Initially we fed her my pumped milk by syringe, per LC recommendations to prevent the dreaded “nipple confusion”—a rejection of the breast altogether that can supposedly occur if bottle-feeding is introduced to a baby too early (standard advice is not sooner than four weeks). But this proved unsustainably time-consuming, so on day 11, we started feeding her pumped milk in a slow-flow bottle. I sobbed because I thought this signaled the end of breastfeeding (spoiler alert: it didn’t), and because being hooked up to a machine and cleaning pump parts eight times a day wasn’t exactly how I’d imagined new motherhood. The skin on my hands cracked from all the soap (and hand sanitizer—thanks, COVID!)

I knew sleep would be in short supply, but didn’t quite realize beforehand that breastfeeding generally means not ever sleeping for more than two hours at a time for at least the first month. When Sahale woke up crying from hunger, my brain would stumble into disoriented consciousness in the dark of our bedroom, only to find my body often soaked in night sweats. Occasionally she’d sleep an extra hour or two and I’d awake with painful breast engorgement—and accompanying milk leakage—that made it feel like someone had beaten me up in my sleep, then hosed me down with cold sweat and milk. (Cute!)
Never before had my body felt so ravaged.
Many wonderful friends delivered meals to us in those early weeks. Touching gifts showed up on our doorstep from all over the world. Family “met” Sahale via Zoom. Friends called and texted to check in. I didn’t always have the time or energy to respond, but their words still meant so much. Those who’ve given birth before checked in with special compassion, acknowledging the depth and intensity of that postpartum fog.
In her memoir, The Blue Jay’s Dance, Louise Erdrich articulates early parenthood well: “Any sublime effort has its dark moments. Perhaps, if anything, the meaning in this book for others may be this: Here is a job in which it is not unusual to be, at the same instant, wildly joyous and profoundly stressed.”

Writing now (at 13 weeks postpartum) about those early weeks feels like recalling a wild dream I had many moons ago. Around one month postpartum (and even more exponentially since then), things began improving. Sahale naturally settled into some semblance of a routine, including longer stretches of sleeping at night. After several weeks of feeding her almost exclusively with pumped breast milk, we finally mastered our latch, thanks to a few fabulous YouTube videos and a couple Zoom sessions with a breastfeeding guru in Alaska named Jen. (Nursing Sahale is now legitimately my favorite part of every day.) The pain in my hip became manageable enough for longer walks and soon, hikes with Sahale in a carrier on my chest.

Returning to Running After My C-Section
My six-week postpartum checkup consisted of little more than a postpartum depression screening (I feel fortunate not to have experienced any symptoms of that), instruction on the importance of postnatal birth control, and a quick check for abdominal wall separation, otherwise known as diastasis recti—something that about 60% of people experience after pregnancy, and which can require special care not to accidentally herniate through by doing crunches or sit-ups, or straining when lifting things (e.g., your baby, cat, laundry basket, etc.) My midwife confirmed I had some lingering abdominal separation—“more than one finger’s width but less than two”—but was pretty breezy about clearing me to start running again.
My first run was 2.5 miles on the treadmill at 4.5mph pace, which felt like sprinting. I spent the whole time terrified that my stomach was going to rip open. (Another spoiler alert: It didn’t.)
Thankfully, running began to feel more comfortable again in the weeks that followed. I mostly run on our treadmill at home, but have ventured out for short trail runs a few times so far. I also try to hike with Sahale a couple times a week.

Downhill running still feels wonky, like my organs are sloshing around inside of me, but uphill running (on trails or treadmill) and hiking all feels pretty great at this point—sweaty, low-impact, an old friend I’ve missed tremendously and am ecstatic to be catching up with again.
Postpartum Pelvic Floor Rehab
Still, I’ve been nervous about overdoing it. Among my many fears about pregnancy was one of long-term pelvic floor damage, which a number of people I know (including many runners) have suffered. Although vaginal birth is rougher on this region than Cesarean birth, pregnancy itself—the growing uterus pushing other organs out of its way—can cause serious trauma to the pelvic floor, resulting in long-term issues like urinary or fecal incontinence, back pain and sexual dysfunction/pain during intercourse. Studies suggest that at six weeks postpartum, around 80% of people have some form of pelvic organ prolapse (POP)—when the bladder, uterus or rectum bulges into the vagina—albeit in varying degrees, with milder prolapses (grade 1 or 2) sometimes resolving on their own with enough time and/or dedicated PT, and more severe prolapses (grade 3 or 4) occasionally requiring eventual surgery to address.
Postpartum pelvic floor injury is rarely discussed; no one on my midwife team brought it up, ever, and a physical examination for it is not a standard postpartum practice. Because the symptoms can be embarrassing, many people wind up suffering in silence, having no idea how common these issues are. Those who’ve experienced severe pelvic floor injury often don’t feel comfortable talking about it, out of fear of scaring others away from pregnancy, or of being shamed for complaining instead of just being grateful for their baby.
But the reality is that postpartum trauma is remarkably common, and sometimes permanently debilitating, especially when not addressed through physical therapy. It’s scary shit, especially when you’re someone accustomed to being active, who depends on physical activity to support mental wellbeing.

There is very little information out there about how to return safely to running (let alone the stupid distances I enjoy covering), but plenty of ominous reminders of what a tremendous stress running inflicts on the pelvic floor. I had this gripe about lack of informed guidance during pregnancy as well, since half the internet says, “Running is too high-impact to be a good choice for exercise during pregnancy, especially in the final trimester” and the other half says, “You go girl, be a badass and run right up until you go into labor!” I suspect the truth is somewhere in between because every body is different. (But I also feel frustrated at the generic “just listen to your body and do what feels right” advice; if it’s your first time being pregnant and giving birth, everything about your body at that time feels fairly novel, so your “this-feels-right” barometer gets tossed out the window.)
As for advice on when to return to running postpartum, six weeks is often quipped as reasonable for a no-complications vaginal delivery, though some studies suggest any running before twelve weeks is risky. For C-sections, the recommendations range from two to twelve months. The consensus on running with pelvic organ prolapse seems to be: don’t. Anecdotal cautionary tales of exacerbating pelvic floor damage abound on runners’ blogs.
I didn’t have any real symptoms of pelvic floor injuries, but I was anxious about them showing up spontaneously by running too much too soon. (Not that I’ve ever been prone to excess when it comes to running. HAHA.) The experiences of many runners I know made me hyper-aware of the risks—so I made an appointment to get evaluated by a pelvic floor physical therapist and enlist professional help in returning to the activities I love. Pray tell, why is this kind of evaluation and support not part of standard postpartum care in America?
At nine weeks postpartum, I was diagnosed at the PT clinic with a grade 1 prolapse—which, again, is super common at this stage and not always symptomatic. Fortunately, I now visit an awesome pelvic floor PT once a week for both internal and external work (plus exercises I do at home three times a week) and monitoring of my body as I slowly rebuild mileage and reincorporate strength training. Pelvic floor rehab is a tricky science; weakness can be an issue, but so can too much tightness. Like many runners, my pelvic floor is more in need of relaxing than it is further strengthening; though kegels are often blanket-recommended both pre- and postnatally, it turns out they’re not actually a great idea if your pelvic floor is already overly tight, which is what makes individual evaluation by a pelvic floor PT or specialized doctor so important.

Coincidentally, my PT also gave birth to her first baby via C-section earlier this year, so we have some things in common. I enjoy chatting with her, even if it is a little awkward to get to know someone while their hand is up your vagina each week. Scar mobilization is also a whole thing that I don’t recall any medical provider at the hospital (neither my midwives nor the nurses or OB who ultimately delivered our baby) ever mentioning to me. I’ve learned about it primarily through Instagram resources and now my PT; the work she’s helped me do to promote proper healing of my scar has already made a huge difference.
(On a side note, the OB who delivered Sahale was fantastic overall, and I am astounded by how tiny and unobtrusive my scar is. I can’t believe they managed to pull a baby through there just three months ago. Modern medicine can be amazing! Another side note: Instagram has been one of the most fruitful sources of information throughout my pregnancy, childbirth preparation and “fourth trimester.” Sahale is a champion sleeper, and I credit that largely to tips gleaned from the Taking Cara Babies Instagram account. Expecting and Empowered is also great for everything postpartum. And BadAssMotherBirther for childbirth prep. I have so much gratitude for those who’ve created these free resources.)
Nevertheless, our society’s healthcare standards for perinatal wellness and postpartum care are inexcusably bad—and socioeconomic and racial disparities only exacerbate this. (If you want to learn more or donate some money to a worthy cause, check out Every Mother Counts.) In my next lifetime, I’d like to open up a nationwide franchise of pay-what-you-can pelvic floor PT clinic/gym combos with free onsite infant/childcare. Philanthropists and venture capitalists, hit me up.
In the meantime, if sharing my own experiences can help even one new parent (perhaps even my own daughter, someday) feel less alone on this wild planet, or seek help for struggles too often suffered in silence, I’ll be glad I did so. Let’s normalize conversations about postpartum wellness, both mental and physical.
Afterword
Listen: becoming a mama is legitimately my favorite thing I’ve done in my life.

Before George and I decided to try to get pregnant, I had a great deal of ambivalence about having children. Even though I’d always said I wanted to keep the door open to the possibility—and struggled through relationships in my twenties with men who didn’t—I still felt myself grow cold with fear every time George would bring up actually starting to try. I was so scared of pregnancy and childbirth interfering with my running, of motherhood (starting at birth, not just jumping in at the preteen years as I did with George’s kids) disrupting my independence and the comfortable identity I’d built for myself in my adult life.
But I’m glad I listened to George, and to other friends of ours who are parents, who told me the magic of having a child is indescribable. It really is—or, at least, has been for me. The love I feel for Sahale is intoxicating, and the joy she brings is all-consuming.

At this time last year, my friend Lauren texted me to ask what I hoped for in 2020. I spent New Year’s Eve a year ago writing her a long email detailing my intensifying desire to get pregnant after several months of already trying with no luck.
2020 may have been a shit show for the world at large, but I’ll always be grateful that it was the year my biggest dream came true.

P.S. Since Sahale was born, George has taken up photography! Since our favorite mutual hobby—running, duh—is something we take turns doing now, it’s been nice to hike together instead, with both baby and camera gear in tow. I am so proud of him for the passion he’s poured into this pursuit, and grateful to him for taking so many of the beautiful photos in this post.



Thank you so much for sharing your experience and also the IG resources that helped you. Pelvic floor damage is no joke and you never get referred to a PT unless you do your own research. So sad a lot of health insurances don’t cover pelvic floor PTs…
I’m glad you’re out of “4th trimester”, things are only gonna be getting more fun from now (in a good way)!!!!
Thank you, Angelina! It’s true that PT referrals are rare. Even when I asked my midwife about this toward the end of my pregnancy (not because I had any symptoms but because I wanted some guidance to help ensure a safe eventual return to long distance running), she seemed surprised: “Why would you want to see one if you’re not having problems? Have you had problems in the past?” + I’ve been super disappointed to learn pelvic floor PT isn’t covered by many insurance companies. Boo! Here’s to hoping our society figures out the importance of perinatal and postpartum care.
Thank you for sharing your story, and helping to normalize some of the craziness of becoming a mom. It’s quite the journey. Glad you’re easing back into running, I probably got a little over eager too soon and it took longer to fully recover. On the flip side, exercise and running are so essential to my mental health. I was really grateful for those early half hour sneak away times to clear my head, have a moment alone and come back home a better mom and partner.
So glad to see you loving parenting through your posts and words, she’s beautiful.
Echoing my reply here from Instagram: Thank you for taking the time to read and respond! Really appreciate hearing your thoughts. You’re so right about mental health being essential to take care of during this time (well, and always) as well, and like you, I find exercise pretty essential for that. And likewise, it’s been a joy to follow along with you and Chris and Joni! Daughters are such a treasure.
I love that you’ve shared your story! And especially bringing to light the women’s health issues that so often never get discussed.
An ultra friend of mine shared her own experience with POP and is now back running big miles. If anyone wants another resource: https://relentlessforwardcommotion.com/old-habits-new-norms-running-with-pelvic-organ-prolapse/
Thank you for taking the time to read and comment, and also to share your friend’s blog! This was definitely one of the blogs I came across when trying to do my research about other runners’ experiences with POP. I so appreciate her sharing so much about her own journey–and, especially, emphasizing the importance of bringing awareness to all (men included) about these all-too-common issues.
Hi Yitka— I found your website after enjoying your piece in the Dec 2020 Trail Runner Magazine about preparing for labor and the unexpected. I was so happy to find this follow-up about your postpartum experience (and pictures of your sweet baby!). Enjoy the journey. I have three (7, 5, and 2) and I also have the strongest core of anyone I know because pelvic floor rehab is never done.
Oh, thank you for taking the time to comment. So glad you enjoyed the essay. Congratulations on your family–three kids, wow! I bow down to you–and I’m glad to hear the core strength can (will?) eventually return. 😀 It’s a slow process, but doing my PT exercises while my baby hops around in her Jolly Jumper next to me has been a great way to build a nice routine around PT.
Cheers to you! Thanks again for reading and commenting. It’s always wonderful to hear from readers of Trail Runner.
A friend just told me about your blog post. I gave up all social media so I am way out of the loop these days! Thank you for sharing your journey. I am 6 months pregnant and you talking through so many of these issues is so helpful for my fears. We got pregnant on the first try…thinking we would have more time! It was a shocker and honestly felt so scary. However, I didn’t want to complain because I know so many struggle. We are so very excited, but there is so much that is fear provoking in this unknown chapter. I appreciate your acknowledgments of being nervous to be a parent, how hard pregnancy and new “momhood” is on your body. It made me tear up a bit reading your brutal honesty in those first weeks. I felt solidarity with you and your words help make me feel more prepared to face the journey ahead with compassion for myself.
Yay, congratulations to you! What wonderful news. (Also, yay for giving up social media! Good riddance, methinks. I’ve taken long breaks from it in the past, and always appreciated the time away.)
Compassion for yourself is the best gift you can grant yourself at this time! Can’t wait to see pictures of your little one when the time comes, and please reach out anytime in your journey if you have questions or just need to rant, cry, explode with happiness, whatever the case may be. It’s a wild ride, but it is the very best one. 😀
Hi Yitka! Congratulations on your beautiful kiddo and thanks for writing this post. I’m five months pregnant, and your description of how you felt about parenthood prior to pregnancy pretty much nails how my husband and I have felt about it … but, like postpartum recovery and prolapse, it’s not something people talk about often, and if you choose your audience wrong (I made that mistake just one time and promptly quit opening my mouth), you get looked at like you’re a monster. The tragedy is that many people do feel ambivalent or uncertain pre-parenthood, and the inability to share is really isolating and can lead to extreme stress and fear. So thank you so much for your honesty and transparency. Hearing that someone I respect felt the same way (and now loves being a mother) is extremely helpful and encouraging. And thanks for all the postpartum recovery tips! Gaining weight and scaling back my running and exercise has been something of an identity and self-esteem crisis for me, and it’s great to see someone who’s passed through the tunnel. And I’m so glad that you and your (slightly larger) family are doing well. 🙂
Hi Katie! I’m a month overdue in replying to your wonderful comment, but congratulations on your pregnancy (and, by now, making it to your third trimester?!) I really appreciated reading all of your thoughts–totally agree that many folks experience ambivalence and uncertainty pre-parenthood, and I’m grateful to all who are willing to share those emotions openly–and hope I get to hear more in the future about your experiences with pregnancy and motherhood.
You might enjoy this film that HOKA recently released on athlete-mom Sophie Power: https://www.youtube.com/watch?v=9QcbaUux5oI
Best wishes with the rest of your pregnancy! Thanks again so much for reaching out. It’s wonderful to hear from you.
Thank you for sharing your story.